Days 9, 10, 11 – Respiratory Distress | Jessica Bussert | Founder & CEO Wednesday, April 22nd
After my last entry I had a free day to myself. I had some errands to run and some shopping to do, so I used the time to catch up. It was a beautiful day in Brooklyn and so I walked to my various appointments and enjoyed a little bit of sunshine for a change. When I’m in a new place I like to take somewhat meandering walks to see other parts of the city and to help better orient myself to where things are. While out I found a lovely little wine shop and bought a nice bottle of Malbec to go with my dinner. Win!
My weekend was spent back in the hospital where I and the rest of the staff all noticed something strange going on. As I mentioned in a previous post, during non-pandemic times the weekends are sometimes a period of increased injury and illness. Joe from the corner office celebrated his new promotion a little too much the night before. Cindy from down the block broke her arm during her Saturday morning Aikido class. Ali, who works at the bank decided he finally needed to get checked out for that nagging stomach pain. So they all head to the emergency department to get seen. Except, this weekend they didn’t…
It seemed to me and the staff that I worked with that most people were wisely trying to stay away from the hospital.
The department was strangely quiet except for COVID patients and the few people who were suffering from other life-threatening emergencies. Of course, there was some overlap between the two groups but by and large, the ER had fewer patients than any of us would have expected. Now, those that did come in kept us on our toes. Let’s talk about that for a moment.
The rest of this entry is going to get pretty graphic. If you’re dealing with too much anxiety about COVID or you’ve recently experienced the loss of a loved one from the virus you might want to skip the rest of this post.
The normal respiratory rate of a human adult is between 12 and 20 breaths a minute. This goes on day in and day out for an average of over 2 million breaths a year without a rest. That’s a lot of work for your poor diaphragm 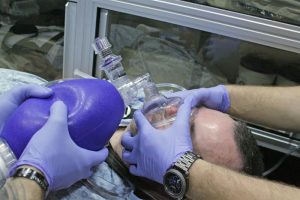 muscle! Now, imagine you’re a long-time smoker or you carry a little too much weight. That’s even more stress on your overworked lungs. And, then, some bozo without a mask coughs in your face and shares their coronavirus with you. Now you’re in real trouble.
muscle! Now, imagine you’re a long-time smoker or you carry a little too much weight. That’s even more stress on your overworked lungs. And, then, some bozo without a mask coughs in your face and shares their coronavirus with you. Now you’re in real trouble.
As the virus invades a person’s lungs it causes inflammation of the tissues and the affected areas begin to ooze fluid and mucus in response. Remember those basic biology classes from back in high school? Your lungs are supposed to act as an air filter, letting oxygen in and carbon dioxide out. Now, imagine taking that filter and covering it with mucus. Breathing becomes a -lot- harder than before.
You can actually check this out with a simple experiment in your own kitchen. Take two coffee filters and drop them partway into a pair of water glasses so they are suspended above the bottom by a few inches. Tape them in place. Now, take some pancake syrup and smear it around one of the filters. Don’t have syrup? Use grape jelly or some other thick substance. Now, gently pour about a cup of water into each filter trying not to disturb the syrup too much. Use your watch to measure how much time it takes the water to filter through each. See how the syrup slows down the transfer of the water in the one glass? That’s what the corona virus does to you. It, and all of the resulting fluid and mucus, slows down the effective transfer of air through the tissues of your lungs.
When someone can’t transfer air effectively they compensate by breathing harder and faster. As I mentioned above, the lungs are already tasked with a lot of work even in the best of times. A bad viral infection will easily double or triple the amount of work the diaphragm muscle needs to do. This is called respiratory distress. Then, after a day or two of too much exertion the tired-out muscle just stops working. The patient will go from huffing and puffing about 40 times a minute to not breathing at all in just a few moments. This is called respiratory arrest and if something isn’t done very quickly the patient will die.
In the hospital we work hard to prevent this all from happening but sometimes it can’t be helped. When it does, then we need to find other ways to breathe for the patient until they get healthy enough to do it on their own once again. The first intervention we use is to manually breathe for them using something called a bag-valve-mask or simply a BVM. In the movies when a doctor or nurse yells out, “They’ve gone into arrest! Hurry up and start bagging them!”, this is what they are talking about. It’s basically just a mask that fits snugly over the mouth and nose with a bag that allows the rescuer to manually push air in and out of the patient’s lungs. We keep bagging the patient until a more advanced airway can be used and the patient can be placed on a ventilator.
Respiratory arrest is the single biggest risk to COVID patients. Unfortunately, sometimes there is just too much fluid and other crud in someone’s lungs for even a ventilator to do the job well enough. And that’s when we lose them.
What can you learn from all of that above? If you see a family member with flu-like symptoms and they are struggling to breathe, don’t mess around. Call an ambulance and get them to the hospital quickly. People move from distress to arrest quickly and with little warning. Even in a well equipped hospital we sometimes lose them. You don’t have the skills or resources to deal with it on your own. Get them to the hospital!
After a weekend dealing with those kinds of issues I was ready for a break. Luckily, after my shift ended Sunday night I wasn’t scheduled back until Wednesday morning. Where is that bottle of wine?